- Augusta University
- Colleges & Schools
- Medical College of Georgia
- Pediatrics
- Allergy-Immunology Fellowship
- Selner's Rhinolaryngoscopy Online
- Selner's Rhinolaryngoscopy Online
Selner's Rhinolaryngoscopy Online

John C. Selner, MD
William K. Dolen, MD
Bryan Spofford, MD
Jerald W. Koepke, MD
Chapter 2. EXAMINATION TECHNIQUE
The physician interested in extending his knowledge of the nose, the pharynx, and the larynx can use fiberoptic rhinoscopy for examination of virtually all patients with upper airway complaints. There are, of course, certain limitations when it comes to examination of children, but with a reassuring bedside manner, proper and safe restraint techniques, and judicious use of analgesics, amnesics and sedatives, examination of even very small children can be accomplished.
PREPARATION FOR EXAMINATION
Other than explanation of the procedure to the patient, the only special preparation usually required is decongestion and anesthesia; the patient is not fasted. Decongestion and anesthesia are usually necessary for adequate examination of recessed structures.
The patient is seated in an examining chair, preferably one with an adjustable headrest. A small child may sit in a parent's lap. Before administration of decongestant and anesthesia, the examiner should perform a preliminary speculum inspection of the anterior nasal cavity to determine patency of the nose and to identify pathology which might be visible on routine examination. The patient is then asked to clear secretions from the nose by gentle blowing of the nose; on occasion, saline irrigation may be necessary to clear the nasal passage of mucus and debris.
Different topical decongestants may be used to shrink the nasal mucosa. An effective decongestant mixture is 0.5% cocaine in a 1.0% ephedrine solution; a 4% solution of cocaine produces both decongestion and anesthesia and will not produce psychotropic effects. Use of cocaine, however, requires disciplined record keeping; the physician may be asked to show use records. Conceivably, traces of cocaine could be detected in a urine drug screen performed after the examination. Other topical decongestants such as phenylephrine, oxymetazoline, and xylometazoline produce variable degrees of decongestion. The selected decongestant is delivered by a standard nasal atomizer. Anesthesia of the pharynx and larynx is not necessary. Nasal anesthesia is readily achieved with 4% xylocaine solution, also delivered by a nasal atomizer. The anesthetic has an unpleasant taste, takes a few moments to take effect, and may produce a transient but uncomfortable globus sensation if swallowed. If desired, the rhinoscope may be lubricated with 2% viscous xylocaine or a water based lubricant.
In administering decongestant and anesthetic, it is important to recall that the nasal cavity is relatively small anteriorly and posteriorly with its largest dimension at the midpoint. In general, one or two sprays of each drug should be directed straight back, and the same amount superiorly and posteriorly at about a 45 degree angle.
In the state of Colorado, fiberoptic rhinolaryngoscopy is not considered an invasive examination. It is the only endoscopic procedure which does not require an informed consent statement.
SEQUENCE OF EXAMINATION
EXAMINATION SEQUENCE
Preliminaries
- Explain procedure to patient
- Speculum examination
- Clear secretions from nose; lavage may be necessary
- Decongestion, anesthetic; lubricate endoscope if desired
Nose, nasopharynx
- Nasal vestibule, septum, nasal floor, inferior turbinate, mucosa
- Superior portions of anterior nose
- Nasal roof
- Middle turbinate
- Nasal floor to choana
- Sphenoethmoidal recess (now, or after laryngeal examination)
- Nasopharynx: adenoidal pad; torus-both sides; Rosenmueller's fossa
Pharynx, larynx
- Lateral and posterior pharyngeal walls, soft palate
- Posterior tongue, lingual tonsils
- Epiglottis, vallecula, aryepiglottic folds Arytenoids, associated cartilages, piriform sinuses
- False vocal cords, true cords, ventricles Transglottic look at trachea
- Remaining nasal structures
- Sphenoethmoidal recess
- Middle meatus
- Contralateral nasal cavity
Examination should proceed in a consistent, logical sequence, which may be varied if needed in individual patients. It is usually convenient to examine structures of the anterior nasal cavity first, followed by examination of the pharynx and larynx. The sphenoethmoidal recess and middle meatus are more difficult to examine and may be less well anesthetized than other structures. Thus, they are generally examined last.
The patient is reminded that he may talk to the examiner during the examination. With proper anesthesia, the procedure is not at all painful; the patient should be asked to communicate any discomfort (other than pressure) to the examiner so that the endoscope may be withdrawn from that area. After lubrication, the endoscope is placed into the nasal vestibule. The examiner's left hand is placed against the patient's forehead approximately at the base of the nose, and the thumb and index finger are used to hold the endoscope at the patient's nostril. Because the examining chair has a headrest, this allows the examiner to have some control of the patient's head and also permits the examiner to keep track of variations in the position of the patient's head. Since many patients will tense the frontalis muscle when more sensitive areas of the airway are examined, it is possible to perceive patient discomfort. Also, changes in skin temperature may be an early sign of a vasovagal reaction.
The right hand is used to advance the endoscope into the nasal cavity. The fingers should grasp and support the endoscope, leaving the thumb free to manipulate the tip of the endoscope. The endoscope is maintained in a straight anterior-posterior position, allowing it to adjust to the contours of the nasal passage as it is advanced, perhaps with slight manipulation of the endoscope tip. The endoscope tip may be flexed with the lever controlled by the thumb of the right hand or moved by altering the position of the endoscope in the nasal passage using the index finger and thumb of the left hand. It is important to remember that, in general, the endoscope will travel towards whatever structure is in the center of the eyepiece or video screen as it is advanced, and that slight flexing or moving the endoscope tip can result in a marked change in the direction of travel. All movements should be performed gently, and the endoscope should not be advanced when distant structures are not visible. Rather than advance blindly, the examiner should withdraw the endoscope slightly, until anatomic landmarks can be seen and recognized.
|
With the endoscope approximately 1 cm. into the nose, the nasal vestibule with its vibrissae (hairs) will have been encountered and often a medial protrusion on the floor of the nose (the lateral feet of the medial crura) will be noted. The inferior turbinate, floor of the nose, and septum will be in view (Figure 1). If the endoscope tip is flexed slightly upward, the middle turbinate will be seen in the distance; with upward flexion to 60-90 degrees, the superior portion of the anterior nose (agger nasi) can be evaluated (Figure 1). If the inferior turbinate is large or swollen, it may be necessary to advance the tip of the endoscope over the anterior margin of the inferior turbinate in order to view the middle turbinate. A large maxillary ridge or displaced septal cartilage may similarly impede advancement of the endoscope. With the endoscope placed in the middle portion of the nasal cavity, the roof of the nose may be viewed by directing the endoscope upwards; this is the region of the cribriform plate. It is not usually possible to advance the endoscope towards the superior turbinate from this position. |
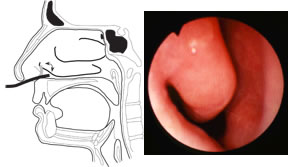
Figure 1. With the endoscope approximately 1 cm. into the nose, the inferior turbinate, floor of the nose, and septum will be in view. If the endoscope tip is flexed slightly upward, the middle turbinate will be seen in the distance; with upward fIexion to 60-90 degrees, the superior portion of the anterior nose (agger nasi) can be evaluated. |
|
In order to view the anterior portion of the middle turbinate, the tip of the endoscope is directed over the inferior turbinate (Figure 2). The endoscope is usually advanced to the choana along the floor of the nose, but this position may be alternatively used if the lower route is obstructed. |

Figure 2. Viewing the anterior portion of the middle turbinate. Note that the tip of the endoscope is directed over the inferior turbinate. While the endoscope is usually advanced to the choana along the floor of the nose, this position may be alternatively used if the lower route is obstructed. |
|
Having been returned to the floor of the nose, the endoscope is directed posteriorly along the nasal floor until it is approximately 4-5 cm. into the nasal fossa (Figure 3). At this point, the choana of the nose (posterior naris) is usually in view, although depending on the size and status of the inferior turbinate, this may not be well visualized. Deviation of the septum may also interfere with observation of the posterior recesses of the nasal fossa. At this point, the tip of the endoscope is directed upward (Figure 3), and the inferior margin of the middle turbinate comes into view. It is usually possible to direct the endoscope superiorly and laterally into the middle meatus either at this point in the examination, or later after examination of the larynx and sphenoethmoidal recess. At this point, identification of the uncinate process and ethmoid bulla, which define the semilunar hiatus, is often possible. The ostium, or accessory ostia, of the maxillary sinus may be identified. The ostia of the nasofrontal duct and the anterior and middle ethmoid air cells are more difficult to locate and ordinarily will not be seen on routine fiberoptic examination of the nose. |
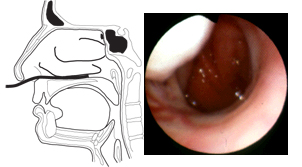 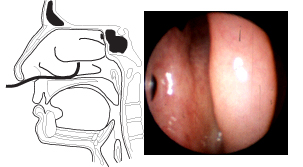
Figure 3. With the endoscope directed posteriorly along the nasal floor, approximately 4-5 cm. into the nasal fossa, one should see the nasal choana (posterior naris) in the distance. When the tip of the endoscope is directed upward, the inferior margin of the middle turbinate comes into view. It may also be possible to direct the endoscope superiorly and laterally into the middle meatus. |
|
Again, the endoscope tip is returned to the floor of the nose and advanced to the posterior margin of the inferior turbinate with the choana clearly in view. It is advanced slightly so that structures of the nasopharynx may be viewed through the choana. The adenoidal pad appears on the posterior wall of the nasopharynx, and the torus tubarius which surrounds the orifice of the eustachian tube is well visualized. The endoscope is advanced into the nasopharynx. Once the posterior margin of the septum (vomer) is lost from view, the tip of the endoscope may be flexed and rotated 90 degrees toward the ipsilateral torus to examine the eustachian tube orifice. The patient may be asked to sing "eeee" or say "k-k-k-k" to make the orifice more visible. If the endoscope is advanced slightly into the nasopharynx and the tip is flexed 180 degrees behind the septum, the contralateral eustachian tube orifice may be examined. Between the posterior margin of the torus and the adenoidal pad is the potential space known as Rosenmueller's fossa. This space begins at the top of the nasopharynx coincident with the adenoidal tissue and proceeds caudad between the torus and the adenoidal pad into the inferior portion of the nasopharynx. After these structures have been examined, the endoscope is rotated back to midline and the tip is flexed inferiorly. The patient is asked to breathe through the nose in order to keep the soft palate from obstructing the view. The lateral and posterior walls of the pharynx, the soft palate, and uvula are inspected for mucosal irregularities, pulsations, and protrusions into the pharynx. The endoscope is advanced into the oropharynx (Figure 4). Structures of the posterior tongue, the epiglottis, the valleculae, and glossoepiglottic and lateral epiglottic folds are examined. |
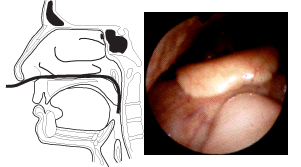
Figure 4. As the endoscope is advanced into the oropharynx, structures of the posterior tongue, the epiglottis, the valleculae, and glossoepiglottic and lateral epiglottic folds are examined. The endoscope is kept close to the posterior wall of the pharynx as it is directed into the hypopharynx. |
|
The endoscope is kept close to the posterior wall of the pharynx as it is directed into the hypopharynx. The patient is encouraged to breathe quietly, and asked not to swallow, but reassured that swallowing will merely result in the sensation of attempting to swallow the endoscope, not in discomfort. In the process of swallowing, the epiglottis can strike the endoscope; should this happen, the endoscope may be withdrawn slightly until the sensation of swallowing the endoscope has been lost. At this point, the examination may continue. The endoscope is directed along the posterior pharyngeal wall in the midline, over the epiglottis (Figure 5). In this position, the arytenoids, the superior projections of the corniculate and cuneiform cartilages, the aryepiglottic folds, the true and false vocal cords, and the ventricles are well visualized. Slight rotations of the endoscope in this position will very clearly reveal the piriform sinuses. From this position, the examiner often will see well into the trachea. |
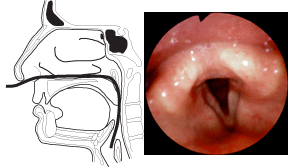
Figure 5. The endoscope is directed along the posterior pharyngeal wall in the midline, over the epiglottis. In this position, the arytenoids, the superior projections of the corniculate and cuneiform cartilages. the aryepiglottic folds, the true and false vocal cords, and the ventricles are well visualized. Slight rotations of the endoscope in this position will very clearly reveal the piriform sinuses. |
|
To examine the cords in adduction, the patient is asked to sing "eeee." Often polypoidal changes and edematous distortion of the vocal cords can be identified with this maneuver. Displacement of the bony structures of the glottis, asymmetrical functioning (including paralysis) of the cords, and pathology such as polypoidal changes, granulomas, contact ulcerations will be apparent at this stage of the examination. Sometimes the endoscope must be withdrawn to just above the epiglottis before the patient is asked to phonate. The endoscope is withdrawn under direct visualization to a position just anterior to the choana. As the endoscope is directed superiorly, the anterior margin of the sphenoid bone comes into view (Figure 6). As the endoscope is advanced superiorly and anteriorly by flexing the tip 90-120 degrees, the posterior and then anterior margins of the superior turbinate may be examined (Figure 6). The sphenoethmoidal recess is medial to the superior turbinate, and the ostium of the sphenoid sinus will often be visualized. The ostia of the posterior ethmoid air cells are less likely to be seen. Since this area may not be well anesthetized in some patients, this portion of the examination may be done after examination of the laryngeal structures. |
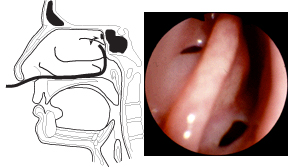
Figure 6. The endoscope is withdrawn to a position just anterior to the choana. As the endoscope is directed superiorly, the anterior margin of the sphenoid bone comes into view. As the endoscope is advanced superiorly and anteriorly by flexing the tip 90-120 degrees, the posterior and then anterior margins of the superior turbinate may be examined. The sphenoethmoidal recess is medial to the superior turbinate, and the ostium of the sphenoid sinus will often be visualized. |
If structures of the middle meatus were not previously examined, they are studied at this time. It is usually easier to examine the middle meatus from posterior to anterior. Following withdrawal of the endoscope under direct visualization, examination of the other side of the nose is carried out. When possible, a videotape of the examination may be replayed and explained to the patient. Afterward, the equipment is cleaned in preparation for the next examination.
In memoriam, John Canty Selner, MD (1936-2006)