Cardiovascular diseases are the leading cause of death in the United States. Understanding the basic and pathological mechanisms underlying cardiovascular disease and searching new ways to prevent and treat cardiovascular disease is a major focus of the Department of Physiology. Faculty in the department study the cardiovascular system from multiple perspectives. The Department offers an advanced Cardiovascular Physiology and Pharmacology course.
Regents' Professor Dr. Michael Brands directs a National Institutes of Health funded Research Program Project Grant examining the role of inflammation in cardiovascular disease.

Zsolt Bagi, MD, PhD - Professor - Physiology
706-721-3423 / zbagi@augusta.edu / CV
Our studies in the Bagi Lab focus on the investigation of the function of small blood vessels. We want to develop a greater understanding of how coronary resistance arteries are controlled in health and disease, and how dysfunction of arteries contribute to organ failure. Our goal is to discover new vascular targets for therapeutic intervention of coronary heart disease and heart failure.

Michael Brands, PhD - Regents' Professor - Physiology
706-721-9785 / mbrands@augusta.edu / CV
Cardiovascular-renal integrative physiology and hypertension. Longstanding interest in renal and hormonal mechanisms for chronic blood pressure and circulatory system control in states of insulin resistance, hyperinsulinemia, and diabetes.

Jessica Filosa, PhD - Professor - Physiology
706-721-8901 / jfilosa@augusta.edu / CV
My major research interest is to gain understanding of the signaling mechanisms governing bi-directional communication among the various cell types within the brain. In particularly, I am interested in the communication between neurons and their surrounding glial and vascular cells. Recent findings have demonstrated an important role for astrocytes as intercellular bridges between the state of neuronal activity and vascular dynamics (or neurovascular coupling). These findings have led to a number of different hypotheses addressing the potential role astrocytes have in neurovascular coupling.

David Mattson, PhD - Department Chair and Professor
706-721-7742 / dmattson@augusta.edu / CV
Studies in the Mattson laboratory examine the normal and pathophysiological regulation of renal function and arterial blood pressure. A particular emphasis is placed on the paracrine, autocrine, and hormonal regulation of renal tubular and vascular function. Additional studies are geared toward an understanding of the genetic basis of hypertension and renal disease.

Paul O'Connor, PhD - Associate Professor - Physiology
706-721-7890 / paoconnor@augusta.edu / CV
Our laboratory’s primary research interests lie in the physiological pathways involved in the regulation of kidney function and how disruptions in these pathways can lead to disease. Recently our laboratory has also become interested in the mechanisms through which splenic anti-inflammatory pathways regulate the innate immune response.

Jennifer Sullivan, PhD - Professor - Physiology
706-721-9796 / jensullivan@augusta.edu / CV
The overall goal of my laboratory is to better understand the molecular mechanisms that regulate blood pressure in males and females under both physiological and pathophysiological conditions, including hypertension. Traditionally, it has been assumed that blood pressure control and the basis of hypertension is the same in males and females; just the magnitude of the response differs. However, based on the vast number of differences that have been identified in cardiovascular physiology, pathophysiology, and pharmacology between the sexes, there is growing evidence to suggest that the pathways by which males and females develop cardiovascular and renal diseases may be distinct. Ongoing studies are focused on 3 pathways involved in blood pressure control and cardiovascular function: the renin angiotensin system (RAS), the nitric oxide (NO) pathway, and inflammation.

Mong-Heng Wang, PhD - Associate Professor - Physiology
706-721-3830 / mwang@augusta.edu / CV
I have worked in the field of cytochrome P450 (CYP)-derived eicosanoids in cardiovascular diseases, renal diseases, and diabetes for more than 20 years. Throughout these years we have identified new compounds and pathways and elucidated their biological activities and their therapeutically potential for treatment of cardiovascular and diabetes-associated disorders.
Science literacy is the artery through which the solutions of tomorrow's problems
flow.
- Neil deGrasse Tyson
Close coordination with members of the Vascular Biology Center and Georgia Prevention Institute ensures a highly collaborative environment.
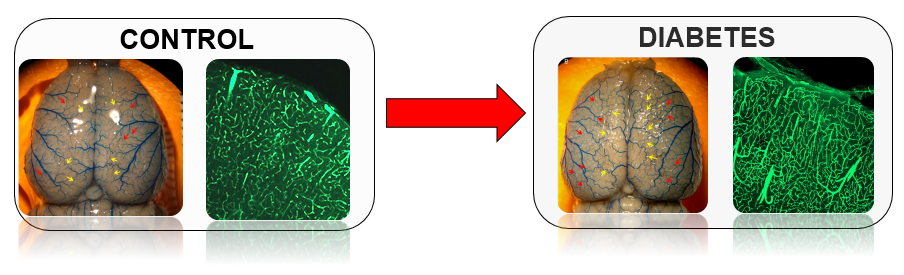 Above: Diabetes promotes excessive yet immature new vessel formation in the brain.
Both the number of collaterals (shown as red and yellow arrows) on the surface of
the brain as well as the vascular density within the brain parenchyma (green dye)
are increased in diabetes. Photo provided by Dr. Adviye Ergul, a former Regents'
Professor with the Department of Physiology.
Above: Diabetes promotes excessive yet immature new vessel formation in the brain.
Both the number of collaterals (shown as red and yellow arrows) on the surface of
the brain as well as the vascular density within the brain parenchyma (green dye)
are increased in diabetes. Photo provided by Dr. Adviye Ergul, a former Regents'
Professor with the Department of Physiology.
